By the time most pregnant women hit 29 weeks, they hit their stride. They have their pregnancy wardrobe down, have mastered the art of sleeping with a body pillow, and speak with their OB/GYN offices more than their friends. But for Stamford Health patient Keri, her third trimester began with an emergency delivery.
Having developed preeclampsia toward the end of her pregnancy with her first child, Keri and her doctors anticipated what to expect the second time around. Preeclampsia is a serious condition typically occurring in the second half of pregnancy. It is usually marked by high blood pressure and protein in the urine. Risk factors include a history of the condition (as Keri had), chronic hypertension, kidney disease, and obesity.
Having developed preeclampsia toward the end of her pregnancy with her first child, Keri and her doctors anticipated what to expect the second time around. Preeclampsia is a serious condition typically occurring in the second half of pregnancy. It is usually marked by high blood pressure and protein in the urine. Risk factors include a history of the condition (as Keri had), chronic hypertension, kidney disease, and obesity.
To treat her preeclampsia, Keri took daily baby aspirin and was monitored more closely by her maternal-fetal medicine specialists. However, as she entered her third trimester, Keri’s blood pressure began rising and growth scans revealed her daughter was on the smaller side. To protect her and her baby, Keri was admitted to the Labor & Delivery Unit at Stamford Hospital. She received a magnesium sulfate drip to prolong the pregnancy and help prevent seizures common with preeclampsia.
The plan was to stay in the hospital until the baby was born, ideally around 34 weeks. While she settled in, Keri felt supported and comforted by the specialists that surrounded her. “All of the nurses were so great,” she said. “One of the doctors from the Cohen Neonatal Intensive Care Unit visited us to explain everything that would happen if we had the baby earlier.”
That evening, Keri’s preeclampsia took a turn. She developed HELLP, characterized by hemolysis or the breakdown of red blood cells, elevated liver enzymes, and a low platelet count. While HELLP is relatively rare in pregnancy (affecting less than 1% of all pregnancies), about 20% of women with preeclampsia develop it during pregnancy.
To treat Keri, her doctors performed an emergency cesarean section.
The plan was to stay in the hospital until the baby was born, ideally around 34 weeks. While she settled in, Keri felt supported and comforted by the specialists that surrounded her. “All of the nurses were so great,” she said. “One of the doctors from the Cohen Neonatal Intensive Care Unit visited us to explain everything that would happen if we had the baby earlier.”
That evening, Keri’s preeclampsia took a turn. She developed HELLP, characterized by hemolysis or the breakdown of red blood cells, elevated liver enzymes, and a low platelet count. While HELLP is relatively rare in pregnancy (affecting less than 1% of all pregnancies), about 20% of women with preeclampsia develop it during pregnancy.
To treat Keri, her doctors performed an emergency cesarean section.
“They immediately swooped into action and did everything they could to keep me calm,” Keri remembered. “The situation was incredibly nerve-wracking, especially seeing so many nurses already in scrubs and being told that blood was ready in case a transfusion was needed. I truly can’t thank Dr. Aksel and the entire team enough for their quick response and care.”
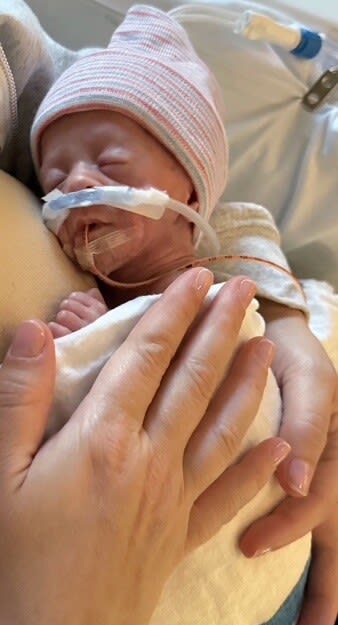
When baby Tatum arrived, she weighed 2 pounds, 2 ounces. As soon as Keri heard her daughter cry, she felt instant relief. “The nurses wrapped her so she stayed warm in the isolette and took a photo of her for us,” she said. “They rolled her over so I could see her, but not being able to hold her right away was tough.”
When baby Tatum arrived, she weighed 2 pounds, 2 ounces. As soon as Keri heard her daughter cry, she felt instant relief. “The nurses wrapped her so she stayed warm in the isolette and took a photo of her for us,” she said. “They rolled her over so I could see her, but not being able to hold her right away was tough.”
Keri recovered at Stamford Hospital for five days and could visit Tatum whenever she wanted to. The recently renovated Stamford Health Cohen NICU is a level III unit and has the latest technology and equipment to care for babies with a low birth weight, respiratory issues, and more.
“It was scary to look at her with all of the wires and CPAP machine. I felt guilty that she was out – and that my body had failed her,” Keri reflected.
As difficult as all those emotions were, Keri was never alone. “The nurses at the NICU are angels on earth,” she said. “They make you feel so comfortable and explain everything to you. I never thought I’d have to leave the hospital without my baby, but I knew that she was in the best care.”
The nurses supported Keri and their family on their NICU journey as well.
“Not only did the nurses provide exceptional care for Tate, treating her as if she were their own, but they also took care of me. They made me feel calm and safe during some of the most overwhelming moments,” Keri elaborated.
“It was scary to look at her with all of the wires and CPAP machine. I felt guilty that she was out – and that my body had failed her,” Keri reflected.
As difficult as all those emotions were, Keri was never alone. “The nurses at the NICU are angels on earth,” she said. “They make you feel so comfortable and explain everything to you. I never thought I’d have to leave the hospital without my baby, but I knew that she was in the best care.”
The nurses supported Keri and their family on their NICU journey as well.
“Not only did the nurses provide exceptional care for Tate, treating her as if she were their own, but they also took care of me. They made me feel calm and safe during some of the most overwhelming moments,” Keri elaborated.
The neonatalogists, pediatric specialists, and nurses estimated the discharge for Tatum around her due date of early December. That meant weeks of juggling her own recovery, keeping the routine at home with her first son, and visiting Tatum at the hospital. “I could call any time I wanted, as much as I wanted, and the nurses were always so happy to speak to me. That made us feel immediately so comfortable with the NICU,” she said.
In the end, Tatum was discharged 68 days after making her entrance to the world. She weighed a healthy 5 pounds on discharge and has continued gaining weight and hitting milestones. But perhaps the best reassurance for Keri and husband, Sammy? Big brother’s stamp of approval: “When we brought her home, he said, ‘She’s so cute.’”
In the end, Tatum was discharged 68 days after making her entrance to the world. She weighed a healthy 5 pounds on discharge and has continued gaining weight and hitting milestones. But perhaps the best reassurance for Keri and husband, Sammy? Big brother’s stamp of approval: “When we brought her home, he said, ‘She’s so cute.’”