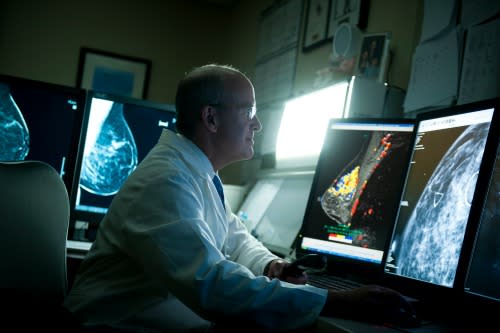
HPV Vaccine Cuts Cervical Cancer Risk By 80%, New Research Finds
Published: January 27, 2026l
Two new reviews confirm that the HPV vaccine is both incredibly effective and safe when given to children before they become sexually active. The findings, published in Britain's Cochrane Review, support the knowledge that we as physicians know: The vaccine has no adverse side effects and prevents the high-risk strains of HPV, or human papillomavirus, from causing cervical cancer in women later in life.
Together, the reviews considered nearly 300 different studies to provide up-to-date research that confirms how critical the HPV vaccine is at preventing cervical cancer. Researchers found that when girls received the vaccination before age 16, they were 80% less likely to develop cervical cancer. As for safety, only short-term side effects like bruising at the injection site were found.
HPV is the most common sexually transmitted infection in the United States. While there are nearly 40 strains of the virus, 13 are high-risk and can lead to several types of cancer such as cervical, vaginal, vulval, and penile.
The HPV vaccine is routinely recommended at age 11 to 12, as a two-dose series. However, for individuals who didn’t receive it before they became sexually active, it can be administered up through age 26. For those older, it’s best to discuss with your physician.
While the Department of Health and Human Services recently removed recommendations for several vaccines for children (including flu, COVID-19, and hepatitis A and B), the HPV vaccination guideline remains unchanged.
The latest findings reinforce previous research and clinical experience with the vaccine since it was introduced in 2006. We know that when compared to a placebo, individual reports of side effects don’t play out. There is simply no data that suggests that the vaccine isn’t safe. And we’ve seen over the past 20 years that when people have utilized the vaccine, there is a significant reduction in cases of cervical cancer.
Historically one major barrier we have with the vaccine is parents who question the timing. They may ask, “Is it really necessary to give my child a vaccine to prevent a sexually transmitted infection when they’re not having sex?”
The answer is, in a word, yes. We know without a doubt that the vaccine is highly effective at protecting against certain cancers caused by HPV, especially when given around ages 11 to 12.
As most sexually active people will contract a strain of HPV at some point (often without symptoms), it’s incredibly important to provide this gift of immunity to our children that will last them a lifetime.
Together, the reviews considered nearly 300 different studies to provide up-to-date research that confirms how critical the HPV vaccine is at preventing cervical cancer. Researchers found that when girls received the vaccination before age 16, they were 80% less likely to develop cervical cancer. As for safety, only short-term side effects like bruising at the injection site were found.
HPV is the most common sexually transmitted infection in the United States. While there are nearly 40 strains of the virus, 13 are high-risk and can lead to several types of cancer such as cervical, vaginal, vulval, and penile.
The HPV vaccine is routinely recommended at age 11 to 12, as a two-dose series. However, for individuals who didn’t receive it before they became sexually active, it can be administered up through age 26. For those older, it’s best to discuss with your physician.
While the Department of Health and Human Services recently removed recommendations for several vaccines for children (including flu, COVID-19, and hepatitis A and B), the HPV vaccination guideline remains unchanged.
The latest findings reinforce previous research and clinical experience with the vaccine since it was introduced in 2006. We know that when compared to a placebo, individual reports of side effects don’t play out. There is simply no data that suggests that the vaccine isn’t safe. And we’ve seen over the past 20 years that when people have utilized the vaccine, there is a significant reduction in cases of cervical cancer.
Historically one major barrier we have with the vaccine is parents who question the timing. They may ask, “Is it really necessary to give my child a vaccine to prevent a sexually transmitted infection when they’re not having sex?”
The answer is, in a word, yes. We know without a doubt that the vaccine is highly effective at protecting against certain cancers caused by HPV, especially when given around ages 11 to 12.
As most sexually active people will contract a strain of HPV at some point (often without symptoms), it’s incredibly important to provide this gift of immunity to our children that will last them a lifetime.
Featured Expert/ Author

Stamford Health Medical Group Member




















)




























































)


)

)
)